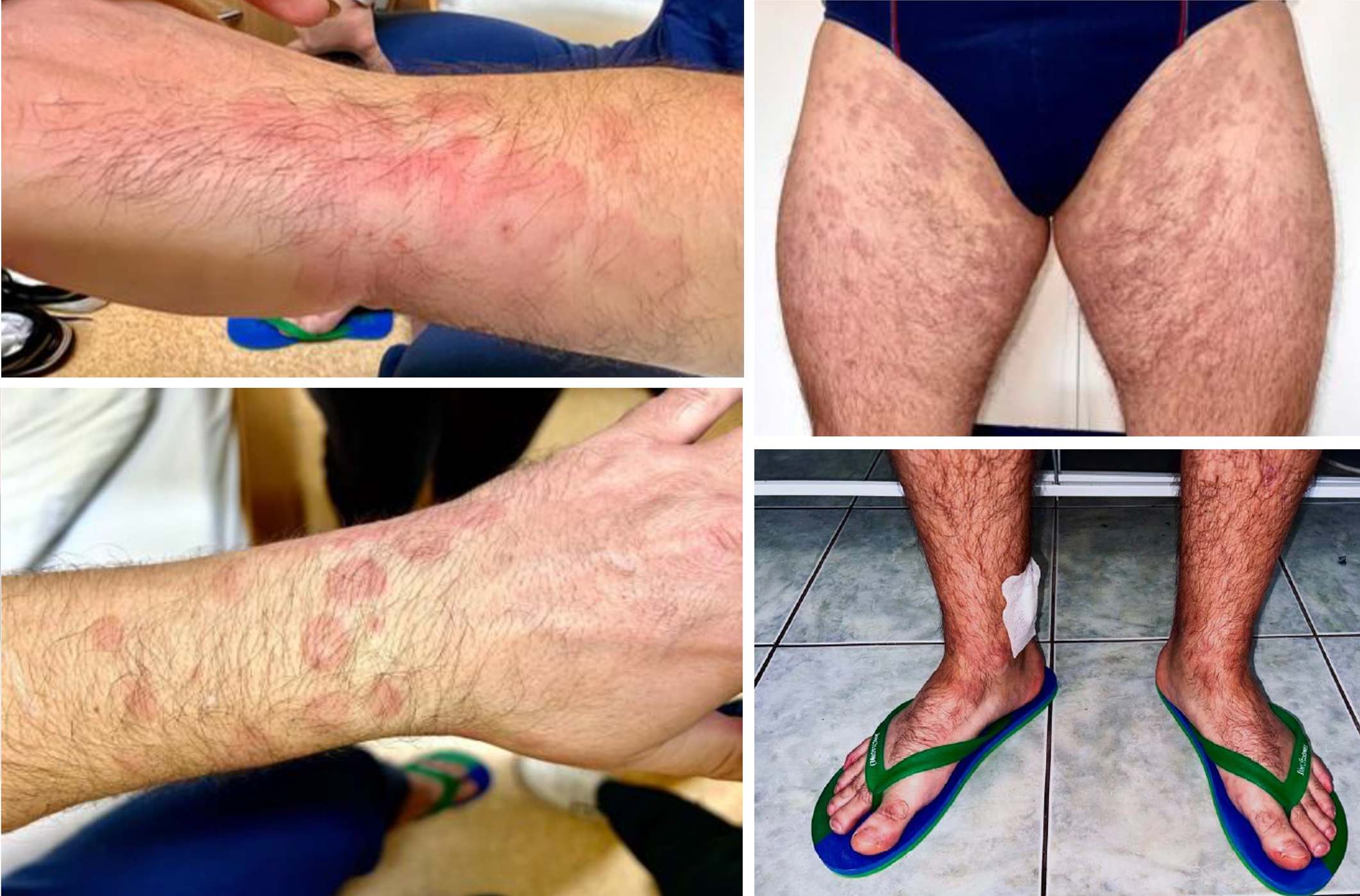
A peculiar clinical presentation of DRESS syndrome
Image Description
Drug-induced exanthemas, the most prevalent cutaneous adverse drug reactions, pose diagnostic challenges due to their diverse manifestations and variable onset.
We describe a case involving a 40-year-old man who exhibited erythematous macules, papules, plaques, and rare target-like lesions symmetrically distributed on his upper and lower extremities. He experienced myalgia, arthralgia, headaches, fever, and flu-like symptoms. Notably, his high serum IgE levels and eosinophilia persisted despite initiating hydrocortisone hemisuccinate treatment two days prior. To establish a diagnosis, we conducted various tests, including screening for viral infections, a skin biopsy, and a peripheral blood smear. We also employed the RegiSCAR DRESS validation scoring system and the EAACI form to identify trigger medications (2,3). Although viral infections could not be identified, uncertainty remained regarding potential influenza exposure while self-administering a combination of metamizole and paracetamol a week before admission. The patient had also been taking pantoprazole, metoclopramide, and sucralfate for six weeks before the exanthema. In our clinic, decreasing systemic corticotherapy led to an increased eosinophil count, which, together with the peripheral blood smear and the biopsy, confirmed DRESS syndrome (1).
The peculiarity of the case presented consists of the patient’s delayed presentation in our clinic, after having received treatment that may have affected all the clinical and paraclinical findings, making diagnosing on purely cutaneous findings and blood tests less reliable, as well as the convoluted history that may indicate triggers for different forms of cutaneous drug reactions (4).
References
Choudhary S, McLeod M, Torchia D, Romanelli P. Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) Syndrome. J Clin Aesthet Dermatol. 2013;6(6):31-37.
Brockow K, Ardern-Jones MR, Mockenhaupt M, et al. EAACI position paper on how to classify cutaneous manifestations of drug hypersensitivity. Allergy. 2019;74(1):14-27. doi:10.1111/all.13562
Sasidharanpillai S, Ajithkumar K, Jishna P, et al. RegiSCAR DRESS (Drug Reaction with Eosinophilia and Systemic Symptoms) Validation Scoring System and Japanese Consensus Group Criteria for Atypical Drug-Induced Hypersensitivity Syndrome (DiHS): A Comparative Analysis. Indian Dermatol Online J. 2022;13(1):40-45. Published 2022 Jan 24.
Fitzpatricks Dermatology in Genereal Medicine, Eighth Edition, 2 Volume set by Lowell Goldsmith, Stephen Katz, Barbara Gilchrest, Amy Paller, David Leffell, Klaus WolffJean L. Bolognia, Julie V. Schaffer, Karynne O. Duncan, Christine J. Ko -Dermatology Essentials-Saunders Elsevier (2014)